Although you may hear otherwise from anti-smoking groups or people with an axe to grind, there is quite a lot of research into the safety of e-cigarettes and their ingredients. A new systematic review from Dr. Konstantinos Farsalinos and Prof. Riccardo Polosa looks at 97 pieces of research on e-cigarettes and their ingredients, providing a comprehensive summary of the body of knowledge to date on e-cigs.
The review addresses the quality of the chemical, toxicological and clinical evidence thus far, as well as weighing up the pros and cons of each approach. In addition, the review also covers issues such as second-hand exposure, accidental nicotine poisonings and the use of e-cigarettes by children.
Summary
- The systematic review of the evidence aims to appraise the chemical, toxicological and clinical safety research to date, as well as addressing related issues such as youth use of e-cigs and the potential risk of “passive” or “second-hand” vaping.
- Chemical research has limitations, but has broadly shown that the majority of harmful constituents of cigarette smoke are absent from e-cig vapor, and where present they are in considerably smaller concentrations.
- Toxicological research conducted using liquids rather than vapor generally produces less favorable results, but the existing research on the vapor shows that the majority of e-liquids are not toxic to cells.
- Clinical research is currently very limited, but provides plenty of evidence of a lack of acute effects from e-cigarette use. Research has reported increased airway resistance, but this is a transient effect which has not been observed in other studies. Additionally, e-cigarettes have been shown to have extremely minor acute effects on the cardiovascular system, if any.
- There is no evidence of a risk to bystanders from e-cig vapor, with all research conducted in ordinary-sized rooms finding nothing of concern. As an illustration of the magnitude of the difference between vaping and smoking, all of the organic carbon emitted from five hours of e-cigarette use would be released from just eleven minutes of smoking.
- Other concerns, such as youth use of e-cigs and potential poisonings, are ultimately unfounded and unsupported by evidence.
- E-cigarettes are much safer than cigarettes, and overregulation would be “an irrational application of the precautionary principle.”
Comparing E-Cigarettes with Tobacco Cigarettes
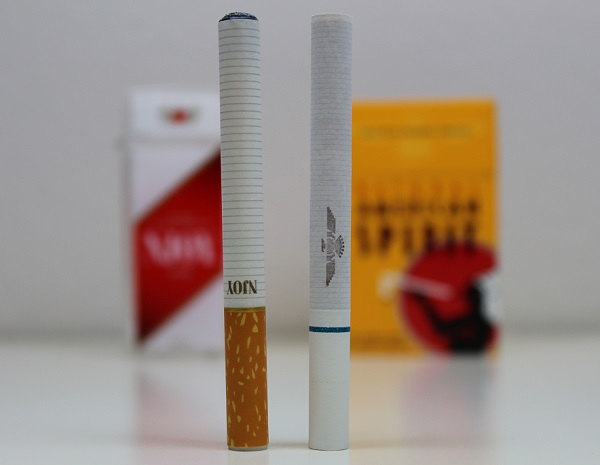
The study (full paper available free if you sign up) specifically addresses the safety of e-cigarettes as a substitute to tobacco cigarettes, and this is an important point noted throughout the paper. The safety of e-cigarettes should be considered in comparison to cigarettes, and they suggest that researchers should always perform comparative tests on cigarette smoke in investigations of vapor (particularly in toxicological studies). This is an extremely important point, because e-cigarettes are intended to be reduced harm products, not absolutely and entirely safe, so their safety should always be measured against the risks of combusted tobacco.
The studies conducted thus far are broken down into three main groups, chemical, toxicological and clinical research, with some discussion of additional issues in separate sections towards the end. To support the evidence specifically addressing e-cigarettes, some older research conducted into their ingredients – such as propylene glycol – is also cited as evidence.
Chemical Studies
Chemical analyses of the contents of vapor are the most common type of research on e-cigarettes, which is essentially because they’re cheap and quick to perform. They’re useful for a theoretical prediction of the likely health impacts of vaping (based on existing knowledge of exposure to toxic or harmful components), but there are many limitations. Researchers only look for specific chemicals (based on those found in tobacco smoke – which may not account for all harmful components), and there isn’t an established protocol for generating the vapor. Also, chemical studies don’t provide direct, objective evidence of the health effects of e-cigarettes in the same way as clinical or – to a lesser extent – toxicological studies. An additional problem identified by the researchers is that while a chemical may be well-known through its use in food, the effects of inhalation may be different from ordinary consumption.
With that said, there have been numerous studies investigating the chemical components of vapor, and they do offer a general picture of the likely health effects of vaping. There is an important distinction drawn, however, between studies which focus on the contents in liquid form or in vapor form. Since different ingredients are vaporized at different temperatures, there is likely to be a difference between what’s found in the liquid and what’s found in the vapor.
Overall, chemical analyses have widely concluded that levels of toxicants in e-cigarettes are much lower than is found in tobacco cigarettes. The research covered ranges from the FDA’s analysis through to more recent studies looking specifically at things like heavy metal content. One of the biggest concerns is the presence of tobacco-specific nitrosamines in e-cigarettes (which are carcinogens). The researchers point to a study conducted in South Korea which found that out of 105 e-liquids, the mean nitrosamine content per ml was just under 13 nanograms. This means that daily exposure from e-cig use is similar to that from patches and gums, and up to 1,800 times less than from a day of smoking. This is the largest piece of research addressing this issue, but the finding is in agreement with numerous other studies cited.
Although reviews focusing on several different chemicals have detected very low quantities of metals, one study which focused on metal and silicate emissions found that in some cases they were detected in higher quantities than would be found in a cigarette. However, this research used poor-quality, first-generation cartomizers, and since the coil used to heat liquid (in any e-cig) is metallic, some residue is to be expected. The researchers also note the unrealistic method (with a short “inter-puff” interval) used means that some of the chemical research bears little resemblance to ordinary use. In either case, the levels found wouldn’t pose a risk to the user’s health. Even if all of the vapor was absorbed (which it isn’t, because much is visibly exhaled), the amount of daily exposure to most metals would be between 4 and 40 times less than is allowed in medicinal products as impurities.
Toxicological Studies
Toxicological research looks directly at the effects of e-cigarette vapor on cultured cells, but there is only limited evidence of this type currently available for e-cigarettes. There are many benefits to this style of research (since it looks directly at the effects of vapor on cells), but the researchers point out there are issues with how well the findings from cultured “in vitro” (in glass) cells can be applied to living (in vivo) humans.
The initial piece of research in this area suffered from major flaws – such as testing the liquid rather than the vapor and failing to offer a comparison with cigarette smoke – but found evidence that some e-liquids were cytotoxic (toxic to cells), particularly to stem cells. However, propylene glycol (PG) and vegetable glycerin (VG) were not cytotoxic, and the cytoxicity corresponded to the peaks in flavoring observed in the samples. In addition, the most cytoxic liquid in this research was a flavor concentrate, which is diluted before vaping.
Further research, involving a testing protocol also used for regulatory purposes for medicines, tested the effects of vapor (produced from 21 different e-liquids) on fibroblast cells in comparison to cigarette smoke. They found only one e-liquid produced vapor that was slightly cytotoxic, and the cigarette smoke – by comparison – was highly cytotoxic even at a concentration of 25 percent. A later and similar study lead by Dr. Farsalinos himself found only 4 of 20 liquids tested were cytotoxic to cultured cardiomyoblasts, and three of these were made using “steeped” tobacco leaves. This study also provided additional evidence that PG and VG aren’t toxic to cells, and expectedly found that tobacco smoke was highly cytotoxic. Generally speaking, the authors conclude that the worst toxicological results come when the experiment involves liquid rather than vapor.
The section concludes with an overview of the limited animal studies conducted in the past on components such as PG, with studies on rats, dogs and primates showing no ill effects. People have been concerned about fog machine vapor (which is composed of the same ingredient), but this has only produced irritation and the PG used isn’t pharmaceutical grade, so this is likely of little concern for vaping.
Clinical Studies and Surveys
Clinical trials are an extremely valuable form of research, but are time-consuming and expensive to conduct, and require extensive follow-up periods. Surveys are much simpler and cheaper, but have the issue of often relying on self-reported answers from self-selected participants. The clinical trials conducted thus far have mainly focused on the efficacy of e-cigarettes for quitting smoking, but evidence from reported side effects is presented for their short-term safety. Generally speaking, throat irritation and coughs were the most common side-effect, with nothing serious having been reported.
Some clinical research has specifically addressed short term effects in users, and one of the most well-known is the study which found an increase in airway resistance after e-cig use. This finding has since been contradicted, and in a study which compared e-cigarettes to tobacco cigarettes, only tobacco was found to have an effect on airways. Other studies have shown that e-cigarettes have no acute effect on cardiovascular functioning, with only a slight effect on the lower blood pressure reading being observed after vaping, compared to sustained and significant effects on both readings after smoking.
Second-Hand Vaping

The researchers also go over the existing evidence on “passive” or second-hand vaping. Given the relative safety of e-cigs for first-hand use, it shouldn’t come as much of a surprise that there is virtually no risk at all.
To illustrate, one study looking for formaldehyde emissions actually found that the dominant effect was from the exhaled breath even before vaping, since people exhale formaldehyde in small quantities anyway.
For all organic carbon-based chemicals (such as acrolein and polycyclic aromatic hydrocarbons), the amount you’d be exposed to as a bystander after five hours of vaping in a room is equal to just 11 minutes of smoking.
For heavy metals, the levels when dispersed into a room would be undetectable and wouldn’t pose a health risk. In fact, any research suggesting any potential of risk to bystanders has suffered methodological issues, and in general, there’s nothing to worry about.
E-Cigarettes, Children, Poisonings and Explosions
The paper then covers many miscellaneous issues – such as a study which showed e-cigs may be an effective method of smoking cessation for schizophrenics (who are currently unable to use medical treatments because of potential side effects) – and does a little bit of myth-busting. They detail the extensive evidence that, even without explicit laws banning youth e-cig use in many places, the overwhelming majority of youths who use e-cigs do so because they’re smokers, with use by non-smokers being consistently low across studies. Even the CDC study people got so worried about only found that 0.5 percent of the whole sample were non-smokers who’d tried an e-cig at least once in the 30 days preceding the survey. There is no issue with non-smoking youth starting to vape regularly, and the “gateway” hypothesis has no supporting evidence. The researchers even suggest that the “gateway” e-cigs provide is merely one out of smoking.
On the issue of accidental poisonings, the researchers use the adverse events surveillance system developed by the FDA and data from the California Poison Control System as evidence. According to a 2013 study, the FDA has received 47 reports since 2008, and none of the eight serious events among them were definitively e-cig related. From the California data, there were 35 cases relating to e-cigs from 2010 to 2012 (with 14 children), and 25 of these were accidental exposure. Only five went to the emergency department, and they were all discharged within four hours with nothing other than nausea, dizziness, vomiting and some mouth irritation.
In other words, accidental e-liquid exposure doesn’t seem to be much of an issue either, but the researchers stress the importance of care around high-strength nicotine concentrate and the importance of child-safe caps. However, they also address the inaccuracies recently uncovered with regards to the lethal dose of nicotine. The current figure (around 60 mg to kill an adult) is almost certainly wrong, with recent research suggesting 500 to 1000 mg as a more reasonable estimate.
The issue of e-cig explosions is also addressed with the cripplingly valid point that cell phones, laptops, and any lithium-powered electronics can explode. This isn’t ideal, but such events are extremely rare and possible with a wide range of technological devices. You can’t point the finger at e-cigs specifically.
Conclusion
The paper provides a very readable and informative analysis of the evidence on e-cigs to date, and it’s well worth reading if you want more detail on the findings. They conclude that despite misrepresentation of research being common with e-cigarettes, it is clear that they are considerably safer than smoking, and yet again underline the importance of always weighing their potential risks against the risks of continued smoking.
They suggest regulation to ensure the current situation with regards to youth use (hardly any use by non-smoking youth) is maintained and that e-cig manufacturers use high-quality products which meet safety standards, but stress that the variety of products currently available must be maintained.
Additionally, Dr. Farsalinos and Prof. Polosa see it as important that e-cigarettes are more easily available than tobacco cigarettes – a poignant point that is too rarely repeated. They argue that the evidence to date is sufficient to prevent restrictive regulation caused by “an irrational application of the precautionary principle,” and we can only hope that the regulators pay attention.

